Where Manual Verification Breaks Down
Manual insurance verification creates:
- Long intake delays
- Denied claims
- Incomplete patient records
- Lost revenue opportunities
- Staff burnout
Verify benefits, create the VOB, and push it directly into your CRM — all from one screen, with one click. No phone calls. No duplicate entry. No switching systems.
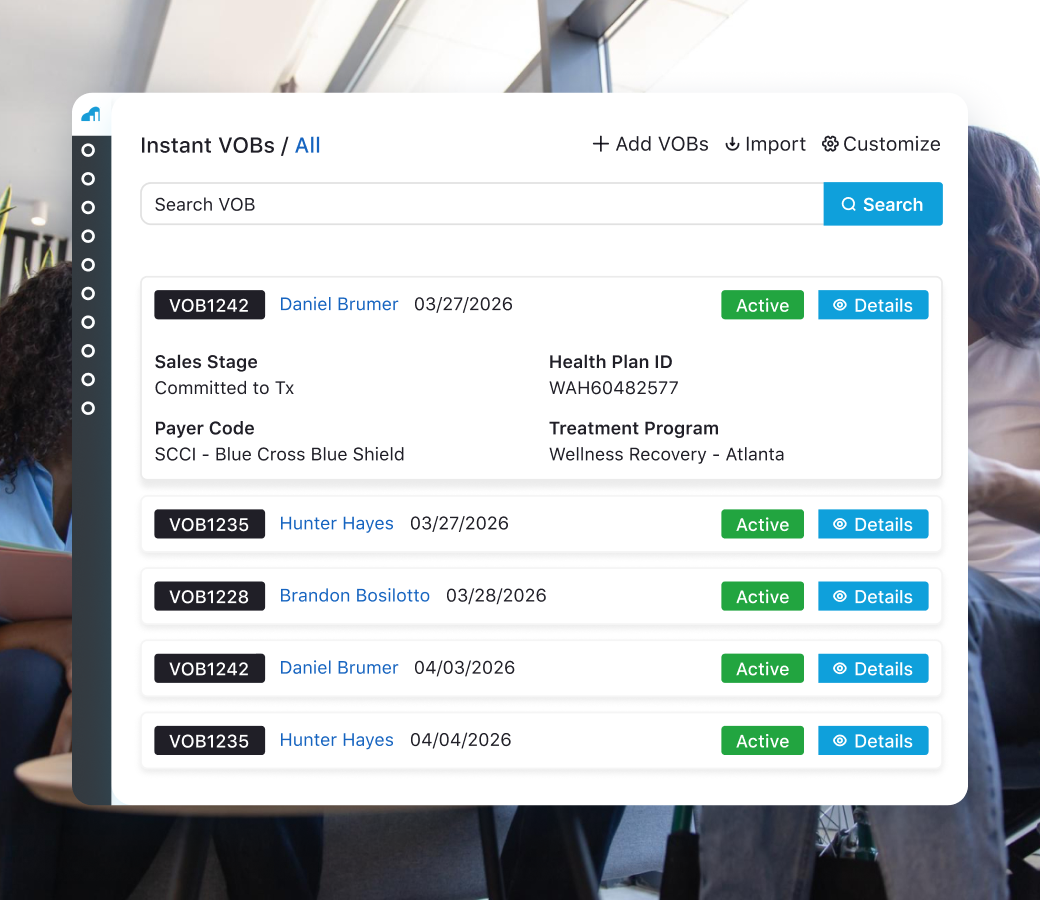
Manual verification slows admissions, drains staff time, and increases the risk of denied claims. iVerify replaces guesswork with instant eligibility clarity.
Manual insurance verification creates:
iVerify automates eligibility checks and pushes clean, real-time results directly into your CRM and billing flow:
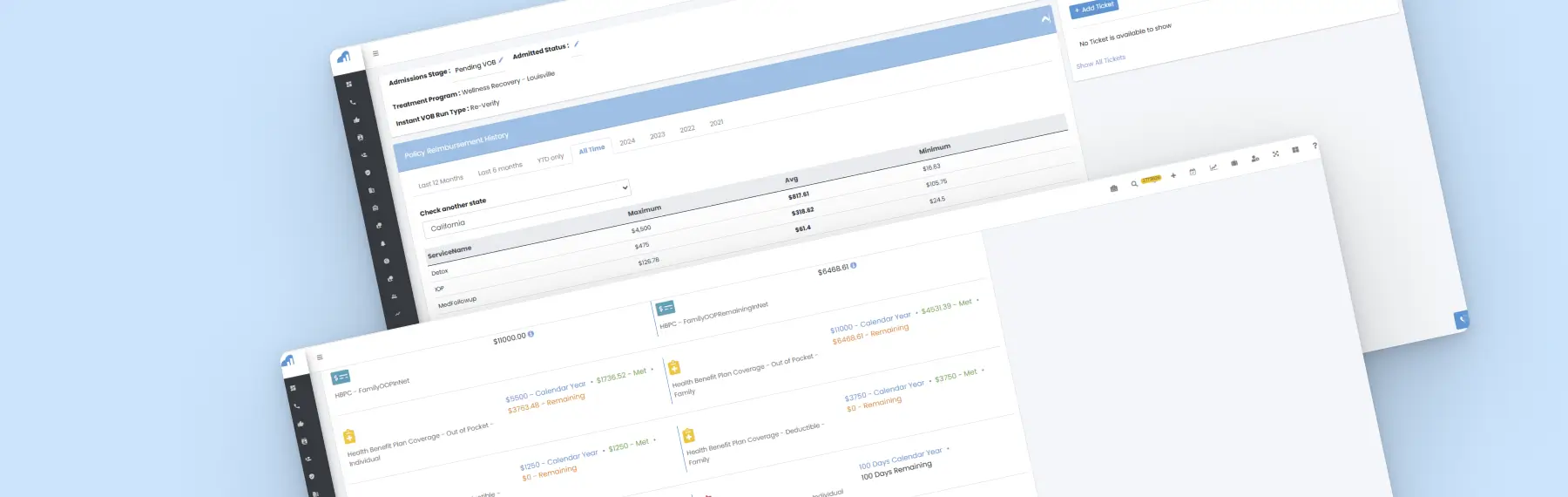
A fast, automated verification workflow designed for behavioral health.
01
Enter patient info
From your Dazos CRM intake record, already pre-populated.
02
Verify with one click
iVerify pings payers and clearinghouses instantly, right inside Dazos.
03
Get a clear answer
Coverage, benefits, copay, OOP maximum, and authorization requirements on one screen.
04
Push to the CRM automatically
iVerify creates the VOB and connects it directly to the patient record. No re-entry, no copy-pasting, no manual handoff.
01
Enter patient info
From your Dazos CRM intake record, already pre-populated.
02
Verify with one click
iVerify pings payers and clearinghouses instantly, right inside Dazos.
03
Get a clear answer
Coverage, benefits, copay, OOP maximum, and authorization requirements on one screen.
04
Push to the CRM automatically
iVerify creates the VOB and connects it directly to the patient record. No re-entry, no copy-pasting, no manual handoff.
iVerify delivers real-time coverage insights, automation, and documentation—built specifically for behavioral health workflows.
Instant verification across national and regional payers, with automatic refreshes for updated benefit changes.
Unlike standalone verification tools that require your team to jump between systems, iVerify lives inside Dazos CRM. Verify a policy, generate a VOB, and attach it to a patient record without ever leaving the platform. One screen. One click. Done.
Clear patient responsibility summaries so admissions teams can set expectations upfront, and alerts when prior authorization is required.
Your business development team doesn’t always verify from a desk. iVerify’s mobile app lets them check benefits from a facility visit, a conference, or anywhere in between.
Push verification results directly into Dazos or your existing EHR with one click—no copy/paste, no double entry.
Every check is saved with a timestamped PDF and a full audit history for billing, appeals, and compliance.
Run eligibility for multiple patients or upcoming appointments at once — perfect for high-volume clinics.
Automatically flags inactive policies, out-of-network plans, or missing information before the patient arrives.
iVerify plugs seamlessly into your existing systems—no workflow redesign, no disruption. Whether you’re running admissions, billing, or clinical operations, Dazos syncs data exactly where your team needs it.
Connects to clearinghouses
Real-time eligibility straight from clearinghouses—no manual lookups.
Syncs with EHRs
Push results directly into your EHR for organized, error-free records.
Ties into intake platforms
Update patient status automatically during intake or pre-admission.
Pushes data into billing
Verified coverage and authorizations flow into billing, reducing denials.
Because iVerify has processed over 12 million behavioral health claims, we can show you something that very few verification tools can: Average Policy Reimbursement history by payer and service type.
See what insurance programs typically pay for the same services:
Real stories from behavioral health leaders.
Streamline admissions, recover revenue, scale alumni engagement and track marketing ROI — all in one platform built for behavioral health facilities.